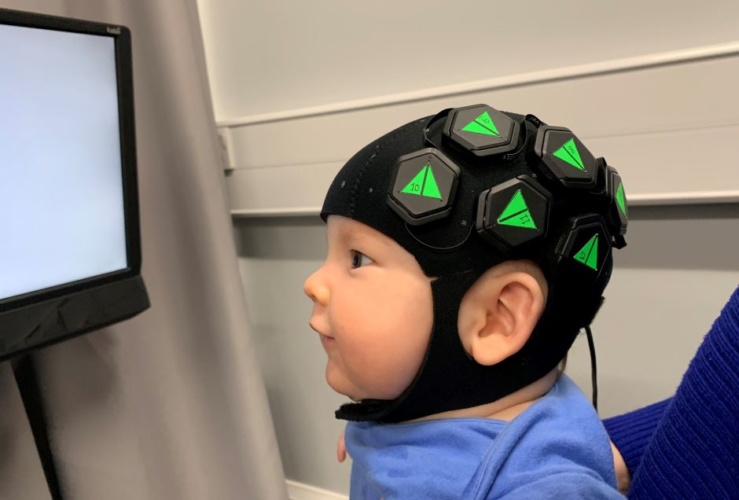
The technology, developed by UCL spinout company Gowerlabs Ltd, is said to use harmless levels of red and near-infrared light delivered via a wearable cap to generate detailed 3D images of babies’ brain activity. It means doctors and neuroscientists can image a baby’s brain without needing MRI, which is expensive and difficult to apply while babies are awake.
It also means researchers can study the infant brain in almost any environment, including in the home.
Microwires and chip record brain activity at scale
Non-invasive brain tech controls robotic arm
In a paper published in NeuroImage, academics and engineers from UCL, Cambridge University, the Rosie Hospital in Cambridge and Gowerlabs Ltd demonstrate the technique - high-density diffuse optical tomography (HD-DOT) - in six-month old infants. The wearable cap employs hundreds of LEDs and optical detectors arranged in a dense network over the scalp to map changes in oxygenation in the brain.
These changes in oxygenation show the areas of the brain that are processing information, meaning the team was were able to create high-quality, 3D images of baby brain activity for the first time outside an MRI scanner.
Project lead Dr Rob Cooper, UCL Medical Physics & Biomedical Engineering, said: “There is a lot we still don’t know about how the brain develops, and a big part of the problem is that studying the infant brain is really difficult with traditional scanners.
“As any parent knows, 6-month old babies are very active; they move around all the time and are easily distracted. Using a technique like MRI, the subject has to remain completely still, which is almost impossible with babies unless they are asleep or sedated.”
Dr Cooper explained via email that current state-of-the-art HD-DOT systems rely on optical fibres to carry light to and from the participant.
“These fibres are heavy and cumbersome and tether the participant to the bench,” he said. “Furthermore, applying enough fibres to make good quality images is really difficult in any participant and nearly impossible in infants.”
He added that the current breakthrough came from Gowerlabs’ Dr. Nick Everdell who realised that to move the electronics to the head, and still allow the devices to be wearable and to conform to the curve of the scalp, required a modular design architecture with multiple independent modules providing emitters and detectors of near-infrared light.
“Multiple modules are then combined to form a network of modules that all talk to each other to produce a dense spider’s web of measurements,” said Dr Cooper. “This is key to allowing these optical devices to produce images of the brain, because the denser the measurements, the better the image resolution.”
In a statement, Elisabetta Maria Frijia, UCL Medical Physics & Biomedical Engineering, who carried out much of the work demonstrating the technology, added: “The approach we have demonstrated is safe, silent and wearable, and can produce images of brain function with better spatial resolution than any other comparable technology.”





Swiss geoengineering start-up targets methane removal
No mention whatsoever about the effect of increased methane levels/iron chloride in the ocean on the pH and chemical properties of the ocean - are we...