Nanotechnologists at Oregon State University’s College of engineering have developed a way of fabricating transparent transistors onto sharply curved surfaces, building on research to develop glucose sensors that can be wrapped around a tube. Although the research was originally directed towards diabetes treatments, and these may be an important application for the technique, it has potential for many other medical applications.
The original research was intended to manufacture a catheter that could be inserted into the bloodstream of a diabetic patient to continuously measure glucose levels. These could then be used to determine the appropriate dose of insulin to be delivered from a pump: effectively, an artificial pancreas. Greg Herman and Xialsong Du had fabricated glucose sensors onto a flat polymer film that was then wrapped around the catheter. In testing, however, the sensors tended to detach from the film, or the film appeal of the catheter.
In their new research, Herman and Du turned to a different method for fabricating sensors: microcontact printing, which uses relief patterns of a “master stamp”, usually made from a soft elastomeric polymer such as polydiimethylsiloxane, to form patterns of layers of ink on a substrate. They use this technique to print amorphous indium gallium zinc oxide field-effect transistors (a-IGZO-FET) directly onto glass tubes with a 1mm radius. They describe the research in a paper in the journal Sensors and Actuators B: Chemical.
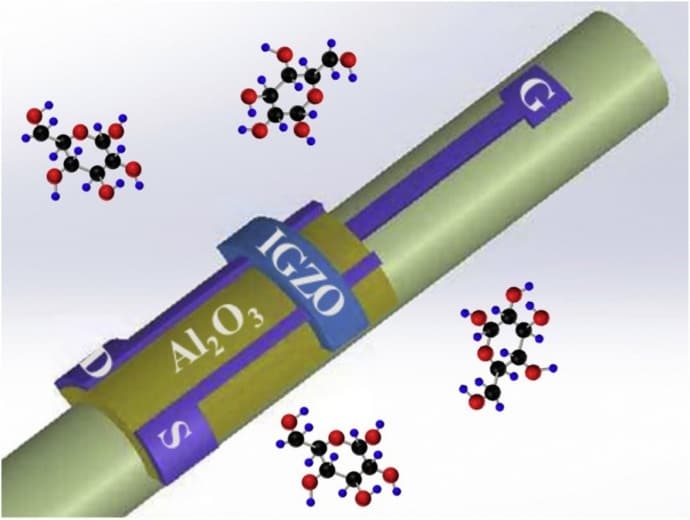
"It takes advantage of an elastomeric stamp's ability to conform to curved substrates with minimal distortion of the printed pattern," Herman said. "The adhesion of the film deposition is very good. For it to come off, you'd essentially have to take a file to it. It's much more rugged than what we had before, and the electronic performance is excellent - it's the same as when fabricated on a flat surface using non-printing methods. We used a glass tube in part to show off the device's transparency." Although simple, the technique had better results than more complex patterning methods such as photolithography or e-beam lithography.
The transparency would not be required for the catheter of an artificial pancreas. However, Herman has experience with transparent sensors – in some recent research, he developed a contact lens equipped with sensors that can detect glucose levels in tears – and he explained that a transparent catheter equipped with transparent sensors could be extremely useful.
“The idea is with a catheter, you could start integrating optical fibres that have the a-IGZO-FET sensors on them," he said. "Some types of sensing need an optical response for detection, so if we can integrate an optical response with an electronic signal, we can expand the detection being done. Field effect sensing may increase the functionality and sensing range of optical sensing systems."
Other applications might be in neural imaging devices, and in endoscopes, which could be made much more sensitive if they incorporated sensing into their imaging capabilities.
For diabetics, particularly Type 1, whose bodies cannot produce insulin at all and who must inject regularly to stay alive, an artificial pancreas would remove the need for frequent blood tests and calculations of appropriate insulin dosage. Increasingly, Type I diabetics use insulin pumps, but currently these are not capable of sensing blood sugar levels.




Red Bull makes hydrogen fuel cell play with AVL
Formula 1 is an anachronistic anomaly where its only cutting edge is in engine development. The rules prohibit any real innovation and there would be...