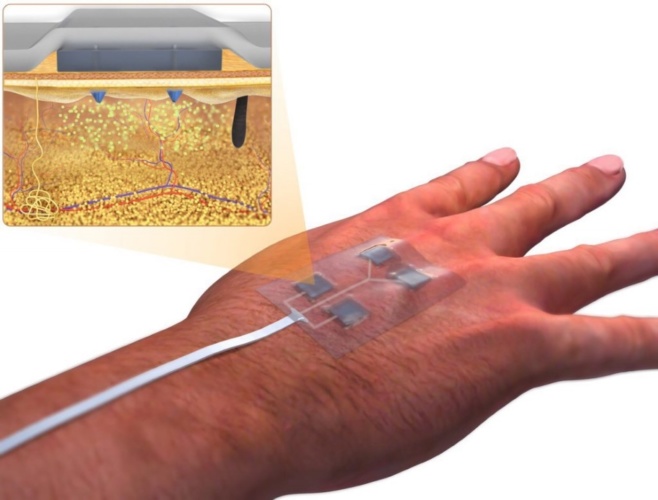
The digital bandage, developed by Dr Ali Tamayol, associate professor, and researchers from the University of Nebraska-Lincoln and Harvard Medical School, is said to be equipped with miniature needles that can be controlled wirelessly, allowing the drugs to be programmed by medical staff without visiting the patient.
New bandage clots blood but doesn’t stick to wound
"This is an important step in engineering advanced bandages that can facilitate the healing of hard to treat wounds. The bandage does not need to be changed continuously," Tamayol said in a statement.
Chronic and non-healing wounds – a complication of diabetes that can lead to limb amputation - affects millions of people each year. Due to the complex nature of these wounds, proper clinical treatment has been limited.
Given the range of processes necessary of wound healing, different medications are needed at different stages of tissue regeneration. Consequently, this requires the development of wearable devices that can deliver agents to critical layers of the wound bed in a minimally invasive way.
With the platform, the healthcare provider can wirelessly control the release of multiple drugs delivered through the miniature needles, which penetrate into deeper layers of the wound bed with minimal pain and inflammation. This method is said to have proved more effective for wound closure and hair growth compared to the topical administration of drugs, and is also minimally invasive.
The research, published in Advanced Functional Materials, was first conducted on cells and later on diabetic mice with full thickness skin injury. With this technology, the mice showed signs of complete healing and lack of scar formation.
These findings, which are subject to a patent application, can potentially replace existing wound care systems and significantly reduce the morbidity of chronic wounds, which will change the way diabetic wounds are treated.




Nanogenerator consumes CO2 to generate electricity
Whoopee, they've solved how to keep a light on but not a lot else.