According to a statement, the system uses an erbium-doped yttrium aluminium garnet (Er:YAG) laser to propel a precise stream of medicine with the correct amount of force.
This type of laser is commonly used by dermatologists, particularly for facial aesthetic treatments, said Jack Yoh, professor of mechanical and aerospace engineering at Seoul National University in South Korea, who developed the device along with his graduate students. Yoh and his team describe the injector in a paper published in the Optical Society’s journal Optics Letters.
The laser is said to be combined with a small adapter that contains the drug to be delivered, in liquid form, plus a chamber containing water that acts as a driving fluid.
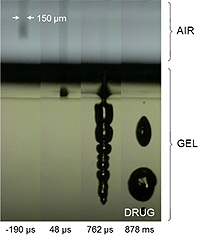
A flexible membrane separates these two liquids. Each laser pulse, which lasts just 250 millionths of a second, generates a vapour bubble inside the driving fluid. The pressure of that bubble puts elastic strain on the membrane, causing the drug to be forcefully ejected from a miniature nozzle in a narrow jet at 150 millionths of a metre in diameter.
‘The impacting jet pressure is higher than the skin tensile strength and thus causes the jet to smoothly penetrate into the targeted depth underneath the skin, without any splashback of the drug,’ Yoh said.
Tests on guinea pig skin show that the drug-laden jet can penetrate up to several millimetres beneath the skin surface, with no damage to the tissue.
Because of the narrowness and quickness of the jet, it should cause little or no pain, Yoh said.
The injection penetrates the epidermal layer, which is located closer to the skin surface at a depth of around 500 micrometres. This region of the skin has no nerve endings, so the method will be completely pain free, said Yoh.
In previous studies, the researchers used a laser wavelength that was not well absorbed by the water of the driving liquid, causing the formation of tiny shock waves that dissipated energy and hampered the formation of the vapour bubble.
In the new work, Yoh and colleagues use a laser with a wavelength of 2,940 nanometres, which is readily absorbed by water. This allows the formation of a larger and more stable vapour bubble, which then induces higher pressure on the membrane, said Yoh.
Although other research groups have developed similar injectors, they are mechanically driven, using piston-like devices to force drugs into the skin, which gives less control over the jet strength and the drug dosage, Yoh said.
‘The laser-driven microjet injector can precisely control dose and the depth of drug penetration underneath the skin. Control via laser power is the major advancement over other devices, I believe,’ he added.
Yoh is now working with a company to produce low-cost replaceable injectors for clinical use.





Swiss geoengineering start-up targets methane removal
No mention whatsoever about the effect of increased methane levels/iron chloride in the ocean on the pH and chemical properties of the ocean - are we...