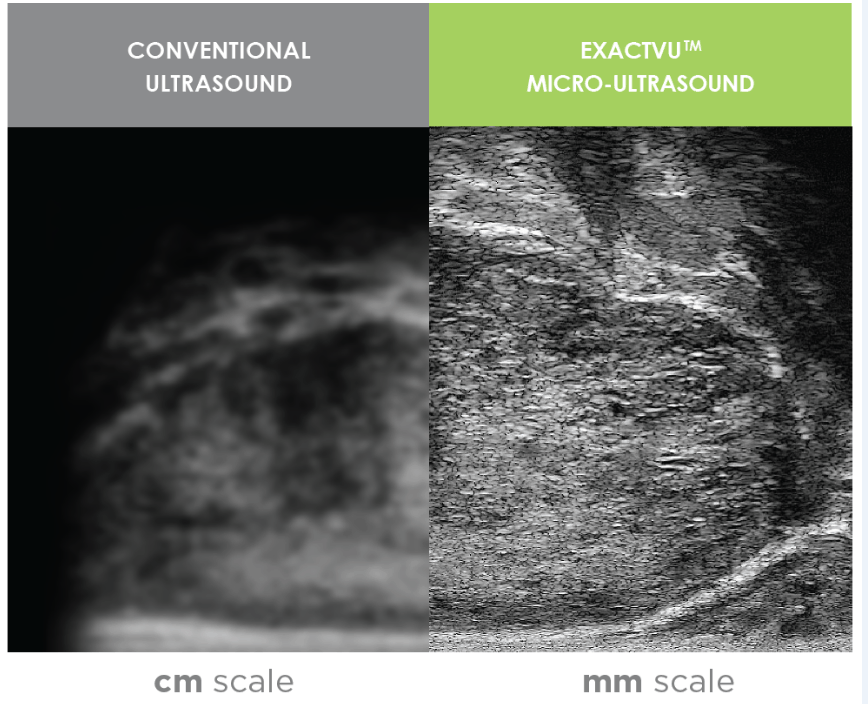
Prostate cancer is the second most common cause of cancer death in men in both the USA and the UK. The current standard-of-care ultrasound, which guides prostatic needle biopsies that help to diagnose prostate cancer, yields a 30 per cent false negative rate as the resolution of the ultrasound systems is insufficient to differentiate suspicious regions.
Operating at 29 MHz, ExactVu is an imaging tool from Toronto-based Exact Imaging that harnesses ultrasound at a microscopic level. It provides a 300 per cent resolution improvement on conventional ultrasound, allowing urologists to better target biopsies for prostate cancer treatment. Exact Imaging has now teamed up with the Cambridge Consultants, the UK technology firm developing an AI to assist with identifying suspicious areas where cancer may be present.
“The AI was trained exclusively on ExactVu images,” Dominic Kelly, machine learning senior consultant at Cambridge Consultants, told The Engineer.
However, as the imaging technology is relatively new, a relatively small dataset of just a few hundred patients was available. This contrasts with the enormous datasets ordinarily used to train neural networks. According to Kelly, this is becoming increasingly common in healthcare, and AI techniques are evolving in order to adapt to the constraints.
“Working with smaller datasets is a common requirement for AI in medical diagnostics and a challenging and important area for research,” he said.
“From our experience developing AI for medical diagnostics we were able to architect an ensemble of deep neural networks which was able to provide high specificity with a relatively small dataset of participant information.”
Cambridge Consultants says the AI analysis should deliver improved accuracy and better characterisation of suspicious regions. The company also claims that its machine learning approach is faster and less computationally intensive than traditional statistical techniques. It says early testing on the proof-on-concept has shown “significant promise” and the system could go on to underpin a commercially-viable software application that enables urologists to make more informed decisions regarding which areas to biopsy. Furthermore, the system could have wider applications in oncology and beyond.
“The most exciting aspect of the system for us, and our research in this area more generally, is its ability to learn the features and characteristics of each problem being tackled,” Kelly explained. “The same system design with only small modification can be trained to identify other forms of cancer and for other forms of diagnostics.”




Nanogenerator consumes CO2 to generate electricity
Whoopee, they've solved how to keep a light on but not a lot else.