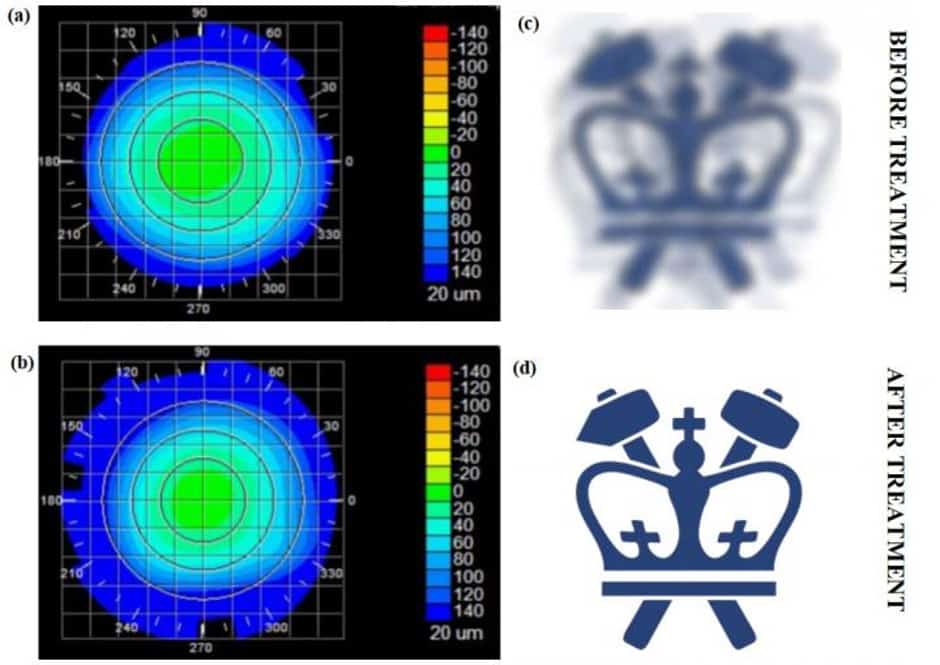
Corneal topography before and after the treatment for myopia, paired with virtual vision that simulates effects of induced refractive power change (credit: Sinisa Vukelic/Columbia Engineering)
Myopia, or near-sightedness, affects 70 to 90 per cent of teenagers and young adults in East Asia alone, and estimates suggest that 2.5 billion people around the world may be affected by the condition by 2020.
Now, Columbia Engineering researcher Sinisa Vukelic has developed a method that uses a femtosecond oscillator - an ultrafast laser that delivers pulses of very low energy - for selective and localised alteration of the biochemical and biomechanical properties of corneal tissue without causing cellular damage and tissue disruption. The study, which could also lead to treatment for hyperopia, astigmatism, and irregular astigmatism, has been published in Nature Photonics.
As well as being non-surgical, the technique is claimed to have fewer side effects and limitations than those seen in refractive surgeries for myopia. Although relatively successful, these surgeries - such as laser in situ keratomileusis (LASIK) and photorefractive keratectomy (PRK) - use ablative technology that can thin and in some cases weaken the cornea. Patients with thin corneas, dry eyes, and other abnormalities cannot undergo refractive surgery.
"We think our study is the first to use this laser output regimen for non-invasive change of corneal curvature or treatment of other clinical problems," said Vukelic.
The technique allows for enough power to induce a low-density plasma within the set focal volume but does not convey enough energy to cause damage to the tissue within the treatment region.
"We've seen low-density plasma in multi-photo imaging where it's been considered an undesired side-effect," Vukelic said. "We were able to transform this side-effect into a viable treatment for enhancing the mechanical properties of collagenous tissues."
According to Columbia, the critical component to Vukelic's approach is that the induction of low-density plasma causes ionisation of water molecules within the cornea. This ionisation creates a reactive oxygen species, which interacts with the collagen fibrils to form chemical bonds, or crosslinks. The selective introduction of these crosslinks induces changes in the mechanical properties of the treated corneal tissue.
When his technique is applied to corneal tissue, the crosslinking alters the collagen properties in the treated regions, and this results in changes in the overall macrostructure of the cornea. The treatment ionises the target molecules within the cornea while avoiding optical breakdown of the corneal tissue. Because the process is photochemical, it does not disrupt tissue and the induced changes remain stable.
"If we carefully tailor these changes, we can adjust the corneal curvature and thus change the refractive power of the eye," said Vukelic. "This is a fundamental departure from the mainstream ultrafast laser treatment that is currently applied in both research and clinical settings and relies on the optical breakdown of the target materials and subsequent cavitation bubble formation."
Vukelic's group is currently building a clinical prototype and plans to start clinical trials by the end of the year.




Red Bull makes hydrogen fuel cell play with AVL
Formula 1 is an anachronistic anomaly where its only cutting edge is in engine development. The rules prohibit any real innovation and there would be...