Despite impressive advances in medical imaging systems, sometimes there is no way to diagnose a disease other than to look inside the body.
This has long been an arduous and unpleasant experience for patients, especially sufferers of digestive disorders. Diagnosing diseases of the upper gastro-intestinal tract — the oesophagus and stomach — can often only be done using endoscopes which patients have to swallow; a process so unpleasant that sedation and anaesthetics are usually needed.
But an easier option is likely to be available soon. Researchers in Israel and Europe are developing a disposable probe containing a tiny camera enclosed in a smooth housing less than an inch across, which doctors will be able to steer around the oesophagus and stomach using a magnetic controller— with little or no discomfort to patients. Even better, the developers believe the system could be cheaper than classical endoscopy.
Swallowable cameras have been used in gastro-intestinal surgery for almost a decade and one of the pioneers in the field, Israeli firm Given Imaging, is one of the partners in the latest research.
The current generation of cameras is housed in passive capsules that cannot be controlled once inside the body. The journey from mouth to stomach takes only four seconds and and cameras simply fall directly to the floor of the stomach.
‘The existing Given Pill-Cam is a good product,’ said Frank Volke of the Fraunhofer Institute for Biomedical Engineering in Sankte Ingbert, Germany, who has developed the steering system for the new camera. ‘It works in the oesophagus to some degree, but not in the stomach because there’s no way to direct it to the region where you need images.
‘It is particularly useful in the intestine and the colon because these are essentially one-dimensional tubes so the body’s peristaltic action moves the camera along smoothly and slowly.’
The results gained from these cameras have been so useful that the EU is sponsoring an important project to develop the technology further. Called NEMO (nano-based capsule endoscopy with Molecular imaging and Optical biopsy), the project has a budget of €4.7m (almost £4m) — of which the EU is providing €2.8m — and combines hardware and biological nanotechnology.
The latter part involves developing ‘nanocontainers’ based on long-chain oily molecules. These carry molecules on their surface that recognise and latch on to malignant cancer cells and contain a dye, which makes these cells visible.
A vital part of the project is a system that can search the gastro-intestinal tract for these dyed areas, and that is where swallowable cameras come in.
Volke’s team is part of a consortium including Given, which is providing the camera and its swallowable housing; and Anglo-Swedish electronics company Zarlink, which is developing a wireless transmission system to transfer images from the camera.
Volke explained that being able to control the camera will allow doctors to diagnose a wider range of diseases. ‘At the moment, if you want to look at the area where there is acid reflux from the stomach which can cause oesophageal cancer, there’s no way to stop a camera and look left and right to study the region in detail — you have to use traditional endoscopy.
‘With the new system, the patient will simply swallow a camera and feel no discomfort as their doctor moves it around.’
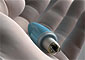
The swallowable camera could soon make inspection of the oesophagus a more pleasant experience for patients
One of the advantages of the consortium is that the existing Given Pill- Cam required minimal redesign, said Volke. The camera is a solid-state LED system surrounded by a ring of cold-light diodes, which emit bright flashes of light several times per second to illuminate areas of interest.
Pictures can then be sent to a display screen for real-time imaging at near-video quality. ‘We can’t take 24 pictures a second but we aren’t far away from that,’ Volke said. Images can also be recorded on a belt-mounted receiver for later viewing. ‘The batteries are included in the camera, the electronics are the same and we use the same housing. All we had to do is make some changes so the camera became magnetically sensitive.’ This is because the steering device, used outside the body, controls the camera via magnetic fields.
The steering device, which was the main focus of Volke’s research, is about the size of a chocolate bar and is moved across the body at a short distance, guiding the camera.
‘The most important thing we had to consider was that the magnetic field was strong enough for us to direct the camera while keeping forces below a certain limit set by the medical team to ensure there was no pain,’ said Volke.
Intellectual property issues prevented Volke from revealing the full details of the steering system but he said the magnetic field is very weak — only 500 milliTesla at the surface of the external manipulator and much weaker at the camera itself.
Steering is effected by a combination of the magnetic force, which is manipulated by moving the steering device through a predefined set of manoeuvres, and the slight friction between the camera and the wall of the oesophagus or stomach.
‘The camera is magnetically sensitive and the external device has north and south magnetic poles,’ said Volke. ‘If you change the position of the external device, the camera follows. But if you constrict the camera’s movement in a tube such as the flexible smooth oesophagus it will try to follow its direction but not have the space, so it will flip round.’
Using this system, the team has been able to move the device up and down, to keep it still and to turn it through 180°.
‘We put a lot of manpower on this project in the early stages to get some good baseline results quickly,’ said Volke. ‘We started with calculations based on simulations and measurements of artificial stomachs and oesophagi, using a variety of distances between the camera and the external device, then recalculated the magnetic fields.’
Tests on pigs followed, conducted by Prof Paul Swain at Imperial College London, to determine the effectiveness of the imaging system and whether it caused discomfort. The results were encouraging so the team went on to a limited human trial — Swain himself swallowed the camera and kept it in his oesophagus for 10 minutes.
‘Paul didn’t experience any discomfort at all, even in this extreme test,’ said Volke. ‘A camera would not usually be in the oesophagus for anything like 10 minutes; a patient would swallow it and the doctor would move it down the oesophagus with the external device, stop at the sensitive point and maybe look left and right to record a couple of images. It would take a maximum of five minutes.
‘But the forces are so minimal and there are no sharp edges on the camera it seems there is no pain. Patients won’t even have to lie down — they could sit in chairs.’
NEMO is a three-year project and although it is only at its halfway point, Volke is confident the results could be seen in hospitals soon. ‘Most of the work on the manoeuvring system has been done and now we need to do more testing on volunteers patients with disorders that have already been confirmed with traditional endoscopy. This is being arranged at the Israelite Hospital in Hamburg,’ he added.
Further developments to the system are likely, including the use of narrow wavebands of light, which enhance the contrast between different types of tissue. But the simplicity of the equipment, the low cost of the camera, the speed of the technique and the lack of anaesthetic could make it an attractive option. ‘It should be cheaper than traditional endoscopy,’ said Volke.




Swiss geoengineering start-up targets methane removal
No mention whatsoever about the effect of increased methane levels/iron chloride in the ocean on the pH and chemical properties of the ocean - are we...