
Just 50 microns in diameter, the sensor has been hailed by the group as a major step forward in the use of an emerging technique known as Microbeam Radiation Therapy (MRT), which promises highly accurate treatment of cancers.
MRT - which uses parallel beams of x-rays, each smaller in diameter than a human hair - is thought to hold particular promise for the treatment of brain tumours, where the risk of damaging surrounding tissues often mitigates against the use of existing radiotherapy treatments.
Until now its use in cancer therapy has been held back by the absence of quality assurance tools that can accurately detect the doses of radiation emitted. But according to research published recently in the journal Scientific Reports the new device - described as a photonic scintillator – provides a solution to this problem.
Commenting on the potential of MRT for cancer treatment, Dr Enbang Li from UOW’s School of Physics said that pre-clinical trials have shown that normal tissue can tolerate peak doses 100 times greater than the doses used in conventional radiotherapy. “An entire tumour could be destroyed with MRT while with significantly reduced damage to adjacent normal tissues,” he said.
He added that whilst the cellular mechanisms behind MRT are currently unknown, it is one of the most promising emerging cancer treatments, particularly for the treatment of brain tumours in children where conventional radiation therapies have a high risk to nervous system development. “MRT represents a new paradigm in radiotherapy and has the potential to become widely available in the future,” he said.
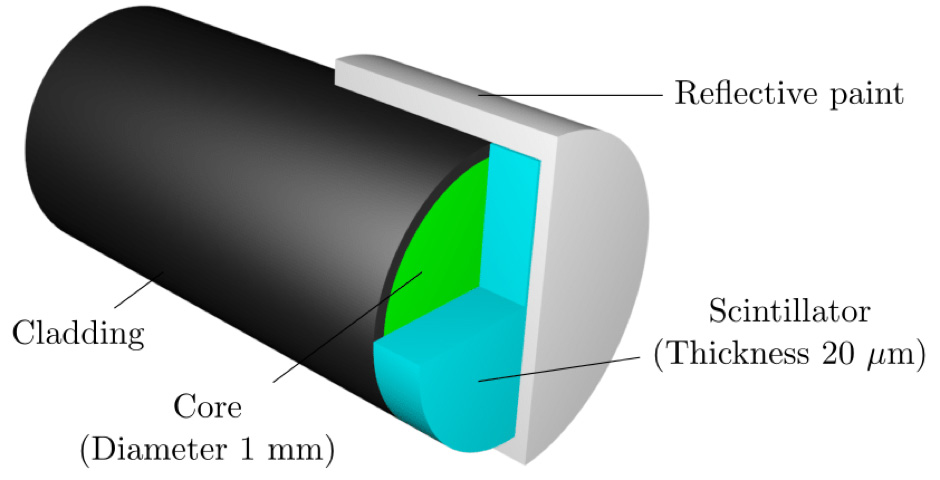
Above: Schematic of the UOW sensor
Li said that that the key challenge in developing the scintillator was making it thin enough to be able to detect the microbeams, but large enough to produce an accurate and reliable measurement signal. “The thickness of the scintillator, or detector, need to be reduced to less than the single beam size, which would significantly reduce the number of photons generated by the scintillator and hence make the photo-detection an extremely challenging task,” he said.
“The results we have achieved so far demonstrate significant steps towards the development of optical dosimeters with the potential to be applied in quality assurance of microbeam radiation therapy, which is vital if clinical trials are to be performed on human patients,” he added.




Glasgow trial explores AR cues for autonomous road safety
They've ploughed into a few vulnerable road users in the past. Making that less likely will make it spectacularly easy to stop the traffic for...