A technique to improve the characteristics of engineered tissues uses ultrasound to align living cells during the biofabrication process, an advance that allows engineered tissue to more closely mimic natural tissues.
The technique from North Carolina State University - ultrasound-assisted biofabrication (UAB) –aligns cells in a three-dimensional matrix during the bioprinting process.
“This allows us to create a knee meniscus, for example, that is more similar to a patient's original meniscus,” said Rohan Shirwaiker, corresponding author of a paper on the work and an associate professor in NC State's Edward P. Fitts Department of Industrial & Systems Engineering. “To date, we've been able to align cells for a range of engineered musculoskeletal tissues."
To align the cells, the researchers built an ultrasound chamber that allows ultrasonic waves to travel across the area where a bioprinter prints living cells. According to NC State, these ultrasonic waves travel in one direction and are then reflected back to their source, creating a ‘standing ultrasound wave.’ The soundwaves effectively herd the cells into rows, which align with areas where the ultrasound waves and the reflected waves cross each other.
"We can control the alignment characteristics of the cells by controlling the parameters of the ultrasound, such as frequency and amplitude," Shirwaiker said.
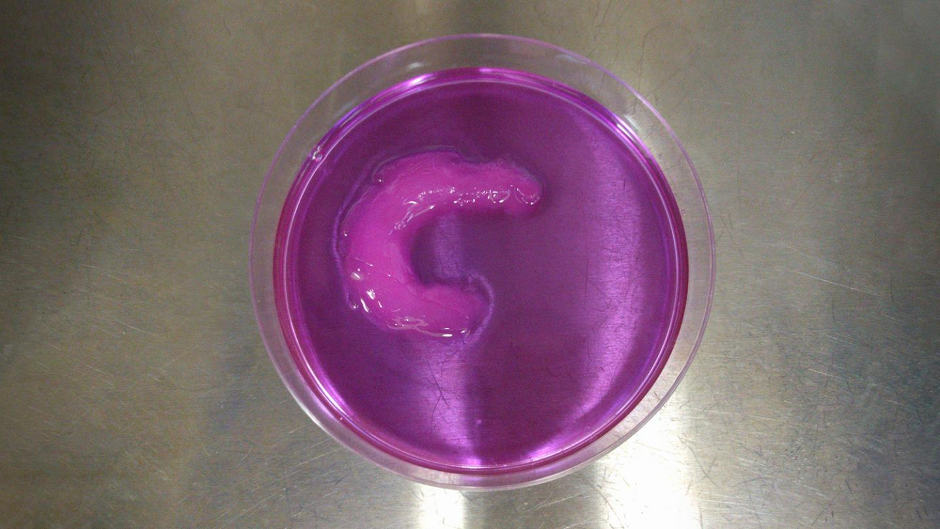
To demonstrate the viability of the UAB technique, the researchers created a knee meniscus with the cells aligned in a semilunar arc.
"We were able to control the alignment of the cells as they were printed, layer by layer, throughout the tissue," Shirwaiker said. "We've also shown the ability to align cells in ways that are particularly important for other orthopaedic soft tissues, such as ligaments and tendons."
The researchers also found that some combinations of ultrasound parameters led to cell death.
"This is important, because it gives us a clear understanding of both what we can do to improve tissue performance and what we need to avoid in order to preserve living cells," Shirwaiker said.
To that end, the researchers have created computational models that allow users to predict the performance of any given set of parameters before beginning the biofabrication process. One other benefit of the UAB technique is that it is relatively inexpensive.
"There's a one-time cost for setting up the ultrasound equipment - which can use off-the-shelf technology," Shirwaiker said. "After that, the operating costs for the ultrasound components are negligible. And the UAB technique can be used in conjunction with most existing bioprinting technologies.”




Red Bull makes hydrogen fuel cell play with AVL
Surely EVs are the best solution for motor sports and for weight / performance dispense with the battery altogether by introducing paired conductors...