
Existing Continuous Glucose Monitors (CGM) measure glucose in interstitial fluid using an invasive sensor with a small needle, which in turn sends data and alarms to a display device. But many patients find this fingerprick testing painful and this can result in low levels of compliance, particularly for children. Using wearable ECG sensors and AI, the Warwick team was able to detect hypoglycaemic events with 82 per cent accuracy, which they claim is comparable to current GCM performance.
How AI is powering a revolution in medical diagnostics
Infrared and AI combine for new brain tumour blood test
"Fingerpicks are never pleasant and in some circumstances are particularly cumbersome,” said Dr Leandro Pecchia, from Warwick’s School of Engineering. “Taking fingerpicks during the night certainly is unpleasant, especially for patients in paediatric age.
"Our innovation consisted in using artificial intelligence for automatic detecting hypoglycaemia via few ECG beats. This is relevant because ECG can be detected in any circumstance, including sleeping."
Published in Scientific Reports, the study details how the AI was trained on the specific patterns of individual patients rather than on cohort data. This is because the ECG signals that correspond to hypoglycaemic events are different for each patient, making it difficult – perhaps impossible – to develop a single AI algorithm that could be rolled out for all patients. While this may restrict the technology to some degree, it will also allow for more tailored treatment of individual patients based on their personal ECG data.
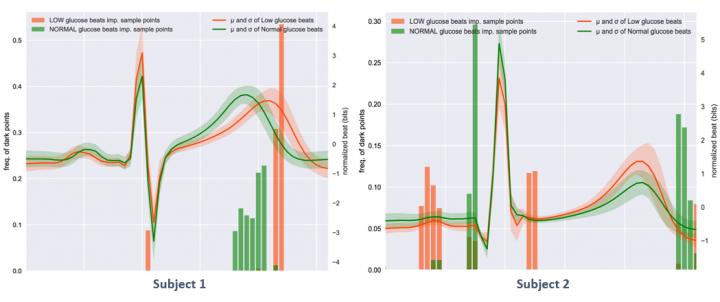
"The differences highlighted above could explain why previous studies using ECG to detect hypoglycaemic events failed,” said Dr Pecchia. “The performance of AI algorithms trained over cohort ECG data would be hindered by these inter-subject differences.
"Our approach enables personalised tuning of detection algorithms and emphasises how hypoglycaemic events affect ECG in individuals. Basing on this information, clinicians can adapt the therapy to each individual. Clearly more clinical research is required to confirm these results in wider populations. This is why we are looking for partners."





Nanogenerator consumes CO2 to generate electricity
Nice to see my my views being backed up by no less a figure than Sabine Hossenfelder https://youtu.be/QoJzs4fA4fo