![Philips_spine def[4]](/media/y5knd330/philips_spine-def4.jpg)
The system, which combines camera images of the outside of the patient with three-dimensional X-rays of the inside of the body, is designed to create a detailed path for the spinal surgeon to follow. This could help to improve surgical tool navigation and implant accuracy, as well as reducing procedure times.
Spinal procedures have traditionally been carried out using open surgery, in which a large incision is made in the body and the muscles moved aside in order to expose the vertebrae.
But this invasive procedure results in a lengthy recovery period and a considerable amount of pain for the patient, according to Ronald Tabaksblat, business leader of image-guided therapy systems at Philips.
However, replacing open surgery with minimally-invasive techniques is particularly difficult in the case of spinal procedures such as vertebrae fusion, as screws are inserted which must be positioned with sub-millimetre accuracy, said Tabaksblat.
“A small error in one direction and you could hit an artery, causing major bleeding, while a small error in another direction means you could hit a nerve, causing nerve damage or even paralysis,” he said.
“This technology is designed to offer the ability to carry out a procedure with a high level of confidence and accuracy, using minimally-invasive techniques.”
The system uses high-resolution optical cameras mounted on a flat-panel X-ray detector to image the surface of the patient. It then combines the external view captured by the cameras with the 3D internal view acquired by the X-ray system to create accurate real-time, augmented-reality images of the patient’s anatomy.
![Philips_spine def2 (1024x683)[13]](/media/vnqhkl12/philips_spine-def2-1024x68313.jpg)
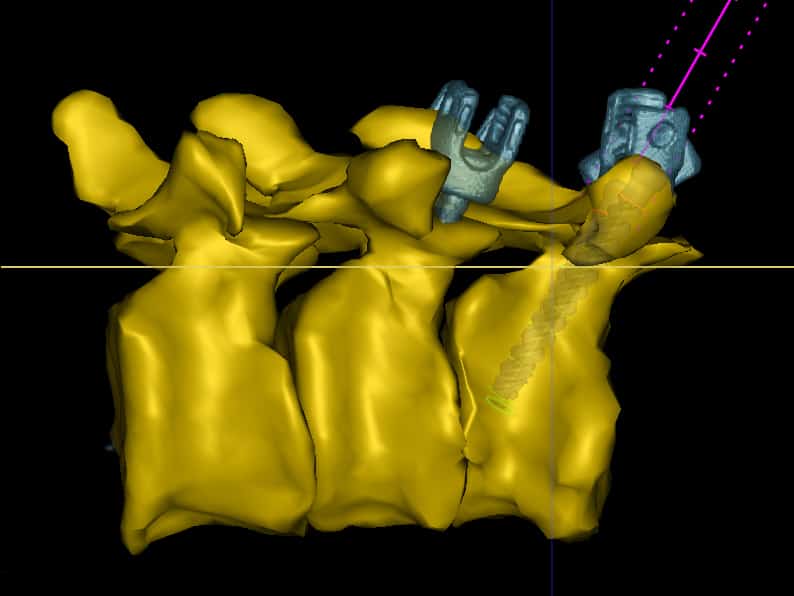
“We can make 3D acquisitions of the vertebrae of the spine, and show where they lie in the body, and we can also register what happens above the skin,” said Tabaksblat. “So now if the surgeon holds an instrument above the skin, we can show them a virtual path along which the instrument should be inserted into the body.”
Small patches stuck onto the patient’s skin are used as landmarks by the software, to ensure it knows exactly where the cameras are pointing in relation to the position of the body at any given time. This also allows it to align the external images with the X-rays of the internal anatomy, and combine the two.
The system generates different 3D views of the patient, from above and to the side, allowing the surgeon to align their instruments accurately before insertion.
The system has undergone pre-clinical trials in an experimental setting at Karolinska University Hospital in Stockholm, Sweden, and the Cincinnati Children’s Hospital Medical Center in the US. In the trials, which were recently published in the journal Spine, the technology was shown to improve the overall accuracy of screw placement from 64 per cent to 84 per cent.
The technology will now undergo clinical trials at 10 hospitals around the world. These will determine whether the system can continue to improve the accuracy of spinal surgery when carried out in a clinical setting.
The company is also investigating the application of the technology in some types of trauma and brain surgery.
Cranial surgery is particularly challenging, as the instant the skull is opened the pressure in the brain is reduced, altering its shape, said Tabaksblat.
“This means any pre-acquired images are pretty much useless once you start operating, so there are significant unmet clinical needs in this area,” he said.




Nanogenerator consumes CO2 to generate electricity
Nice to see my my views being backed up by no less a figure than Sabine Hossenfelder https://youtu.be/QoJzs4fA4fo