Smart textile arm sleeve aims to relieve lymphoedema
Engineers at Nottingham Trent University are leading the development of a smart textile arm sleeve that uses electrical stimulation to reduce swelling and discomfort for patients with lymphoedema.
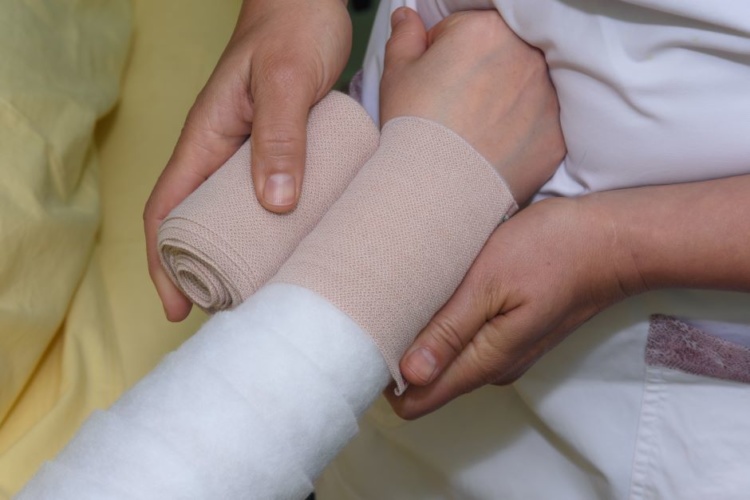
Impacting up to 250 million people globally, lymphoedema is a chronic condition caused by fluid collecting in the soft tissue of the body, usually in the arms or legs with no cure or proven pharmaceutical treatment.
MORE FROM MEDICAL & HEALTHCARE
According to Nottingham Trent, the new sleeve will be a highly-breathable fabric with integrated and flexible printed circuits and electrodes. The circuit (100 micron thick, 5mm wide) will be designed with low power in mind, researchers said, and batteries will be used for patients' ease of use - however, the team said that exploring harvesting energy from body movement or temperature could be a future possibility.
It is being created in partnership with Nottingham University Hospitals NHS Trust and £450,000 in EPSRC funding.
The sleeve – durable and washable, and adapted to fit different patients - will increase circulation of the lymphatic system, which is the network of channels and glands that remove excess fluid in the body.
Register now to continue reading
Thanks for visiting The Engineer. You’ve now reached your monthly limit of news stories. Register for free to unlock unlimited access to all of our news coverage, as well as premium content including opinion, in-depth features and special reports.
Benefits of registering
-
In-depth insights and coverage of key emerging trends
-
Unrestricted access to special reports throughout the year
-
Daily technology news delivered straight to your inbox










Water Sector Talent Exodus Could Cripple The Sector
Maybe if things are essential for the running of a country and we want to pay a fair price we should be running these utilities on a not for profit...