Miniature robot surgeons prepare for cataract surgery
Cambridge Consultants have shown that the procedure to perform cataract surgery could soon be carried out robotically. Helen Knight reports
Cataract surgery is the most commonly performed procedure in the world, restoring sight to 20 million people each year.
But the procedure is currently performed by hand, using a pair of surgical tweezers and a microscope. This can result in complications, as the delicate nature of the surface of the eye means it can be easily damaged.
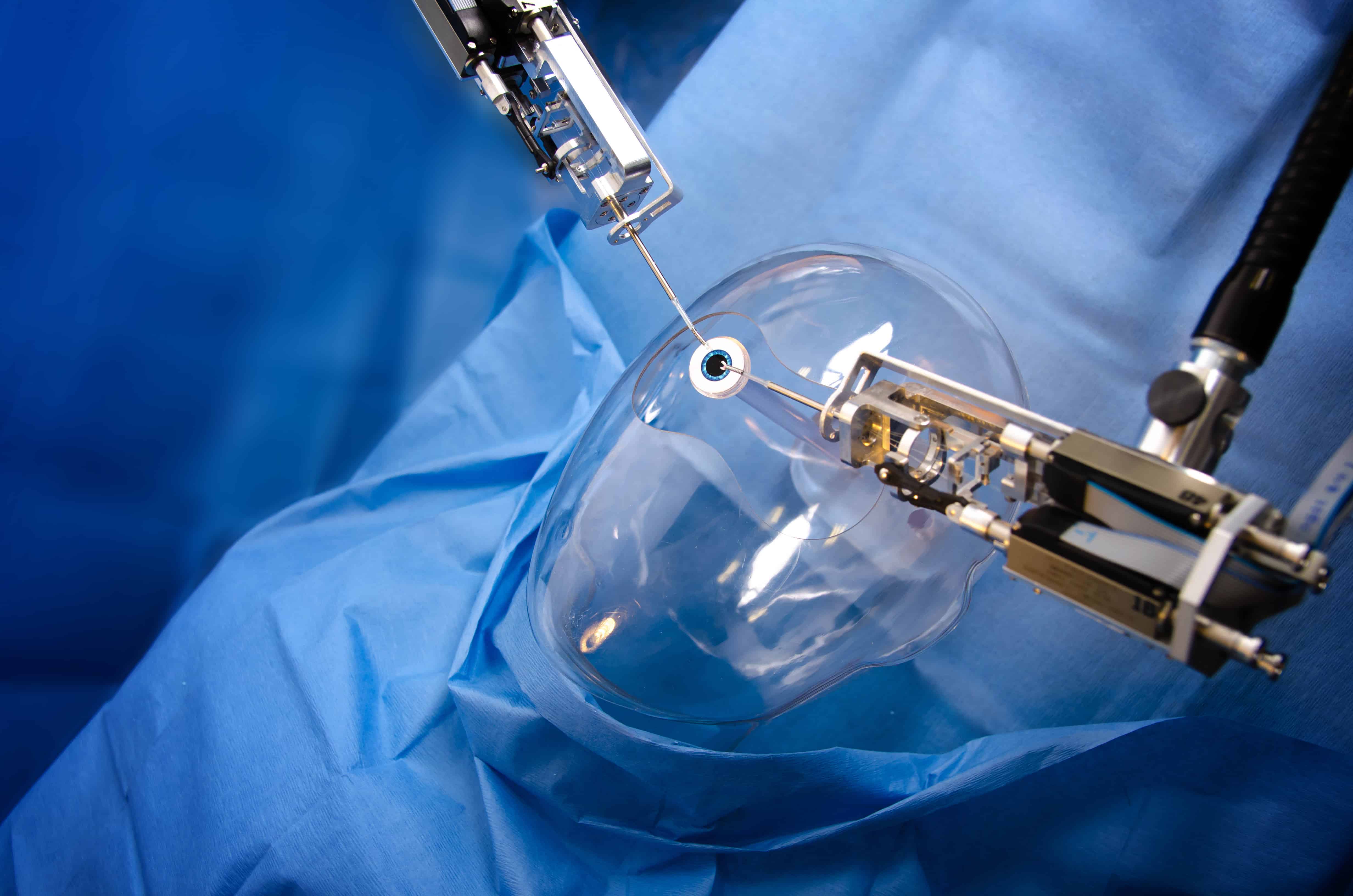
Now engineers at product design firm Cambridge Consultants have shown that the procedure could soon be carried out robotically, thanks to the development of one of the smallest known surgical robots.
Axsis, developed by the company’s engineers to demonstrate the technology’s potential, has a body the size of a soft drinks can, and can manipulate surgical instruments of 1.8mm in diameter.
As well as performing cataract and other forms of eye surgery, the robot could also be used for other minimally invasive procedures, such as implanting neurostimulation devices, early cancer intervention, and oesophageal and gastrointestinal tract operations.
Register now to continue reading
Thanks for visiting The Engineer. You’ve now reached your monthly limit of news stories. Register for free to unlock unlimited access to all of our news coverage, as well as premium content including opinion, in-depth features and special reports.
Benefits of registering
-
In-depth insights and coverage of key emerging trends
-
Unrestricted access to special reports throughout the year
-
Daily technology news delivered straight to your inbox










Water Sector Talent Exodus Could Cripple The Sector
Maybe if things are essential for the running of a country and we want to pay a fair price we should be running these utilities on a not for profit...