In a report published in Biomaterials, a team of scientists at Beth Israel Deaconess Medical Center (BIDMC), the Wyss Institute for Biologically Inspired Engineering and the John A. Paulson School of Engineering and Applied Sciences (SEAS) at Harvard University has demonstrated that the innovative, ultra-low adhesive coating reduced bacterial adhesion by more than 98 per cent in laboratory tests.
"Device related infections remain a significant problem in medicine, burdening society with millions of dollars in health care costs," said Elliot Chaikof, MD, PhD, chair of the Roberta and Stephen R. Weiner Department of Surgery and Surgeon-in-Chief at BIDMC and an associate faculty member at the Wyss Institute. "Antibiotics alone will not solve this problem. We need to use new approaches to minimize the risk of infection, and this strategy is a very important step in that direction."
The self-healing slippery surface coatings - dubbed 'slippery liquid-infused porous surfaces' (SLIPS) - were developed by Joanna Aizenberg, PhD, a Wyss Institute core faculty member, Professor of Chemistry and Chemical Biology and the Amy Smith Berylson Professor of Materials Science at SEAS at Harvard University.
Inspired by the Nepenthes pitcher plant that uses the slippery surface of its leaves to trap insects, Aizenberg engineered surface coatings that repel a variety of substances across a range of temperature, pressure and other environmental conditions. They are said to be stable when exposed to UV light, and are low-cost and simple to manufacture. The current study is the first to demonstrate that SLIPS not only limit the ability of bacteria to adhere to surfaces, but also impede infection in an animal model.
"We are developing SLIPS recipes for a variety of medical applications by working with different medical-grade materials, ensuring the stability of the coating, and carefully pairing the non-fouling properties of the SLIPS materials to specific contaminates, environments and performance requirements," Aizenberg said in a statement. "Here we have extended our repertoire and applied the SLIPS concept very convincingly to medical-grade lubricants, demonstrating its enormous potential in implanted devices prone to bacterial fouling and infection."
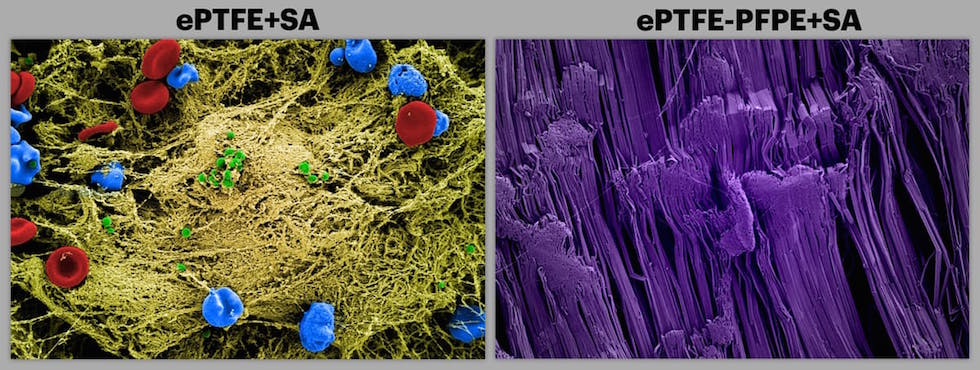
In a series of trials, the researchers tested three SLIPS lubricants for their anti-adhesive qualities. First, they incubated disks of SLIPS-coated medical material ePTFE - a microporous form of Teflon - in Staphylococcus aureus (S. aureus), a bacterium found in the nose and on skin that is one of the most common causes of hospital-acquired infections. After 48 hours, the three variations of SLIPS-treated disks demonstrated 98.3, 99.1 and 99.7 per cent reductions in bacterial adhesion.
To test the material's stability, the scientists performed the same experiment after soaking the SLIPS-coated samples for up to 21 days in a solution meant to simulate conditions inside a living mammal. After exposing these disks to S. aureus for 48 hours, the researchers found nearly 100 per cent reductions in bacterial adhesion.
Widely used clinically, medical mesh is particularly susceptible to bacterial infection. In another set of experiments to test the material's biocompatibility, Chaikof and colleagues implanted small squares of SLIPS-treated mesh into murine models, injecting the site with S. aureus 24 hours later. Three days later, when the researchers removed the implanted mesh, they found little to no infection, compared with an infection rate of more than 90 per cent among controls.





Virgin Atlantic’s Flight100 saved 95 tonnes of CO2 in first SAF flight
LOL a time-honoured unit of volume measurement,, just as large <i>AREAS</i> are expressed as multiples of the size of Wales … or renewable energy...