Everybody knows R2-D2. Such is the success of the Star Wars films that even those with no interest whatsoever in science fiction would recognise the little cylindrical robot on its three legs. They might even know that its stubby body houses a number of delicate manipulators for interfacing with external computers, and carrying out precise tasks. But they might be surprised to find that fiction has begun to leak into reality, because there is now a real R2-D2 that is designed to carry out the most precise tasks. And although the characters in Star Wars trust R2-D2 implicitly, the people who come into contact with its real-world namesake will have to invest an even greater amount of trust in it, because this robot’s job is to maintain and even restore the sense most precious to human beings: eyesight.
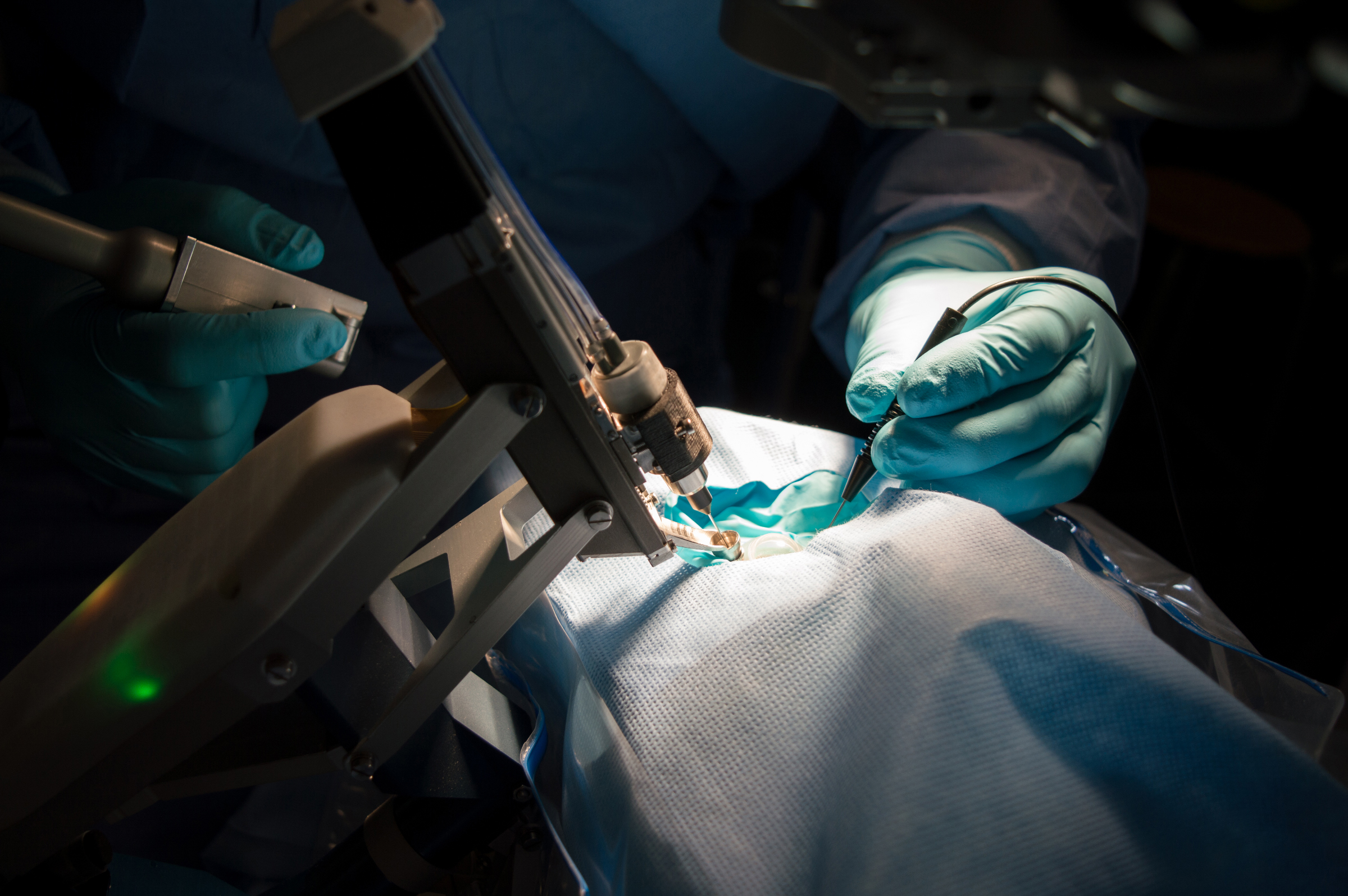
The real-world R2-D2 is a series of trials being carried out by a surgical robot, the Preceyes surgical system (PSS). But unlike its fictional counterpart, this is no clamp-handed humanoid looming over an operating table. Instead, the PSS is a tool intended to assist human surgeons in difficult and arduous procedures. Surgical-assistance robots such as this are a relatively recent addition to the operating theatre, as they are very expensive and not yet in particularly widespread use, but in some fields of surgery they are becoming more accepted and better known.
In The Engineer, for example, we have written about the da Vinci robot, which is used particularly for minimally invasive abdominal surgery and increasingly for heart valve replacement. There are a little over 3,000 da Vinci robots in operation around the world. Like da Vinci, PSS is a tele-operation robot: that is to say it has robotic arms tipped with mechanical manipulators that grasp surgical instruments and carry out the actual procedure; these are controlled by the surgeon using a joystick pad somewhat similar to those used in video games, with software intermediating between the control pad and the manipulators.
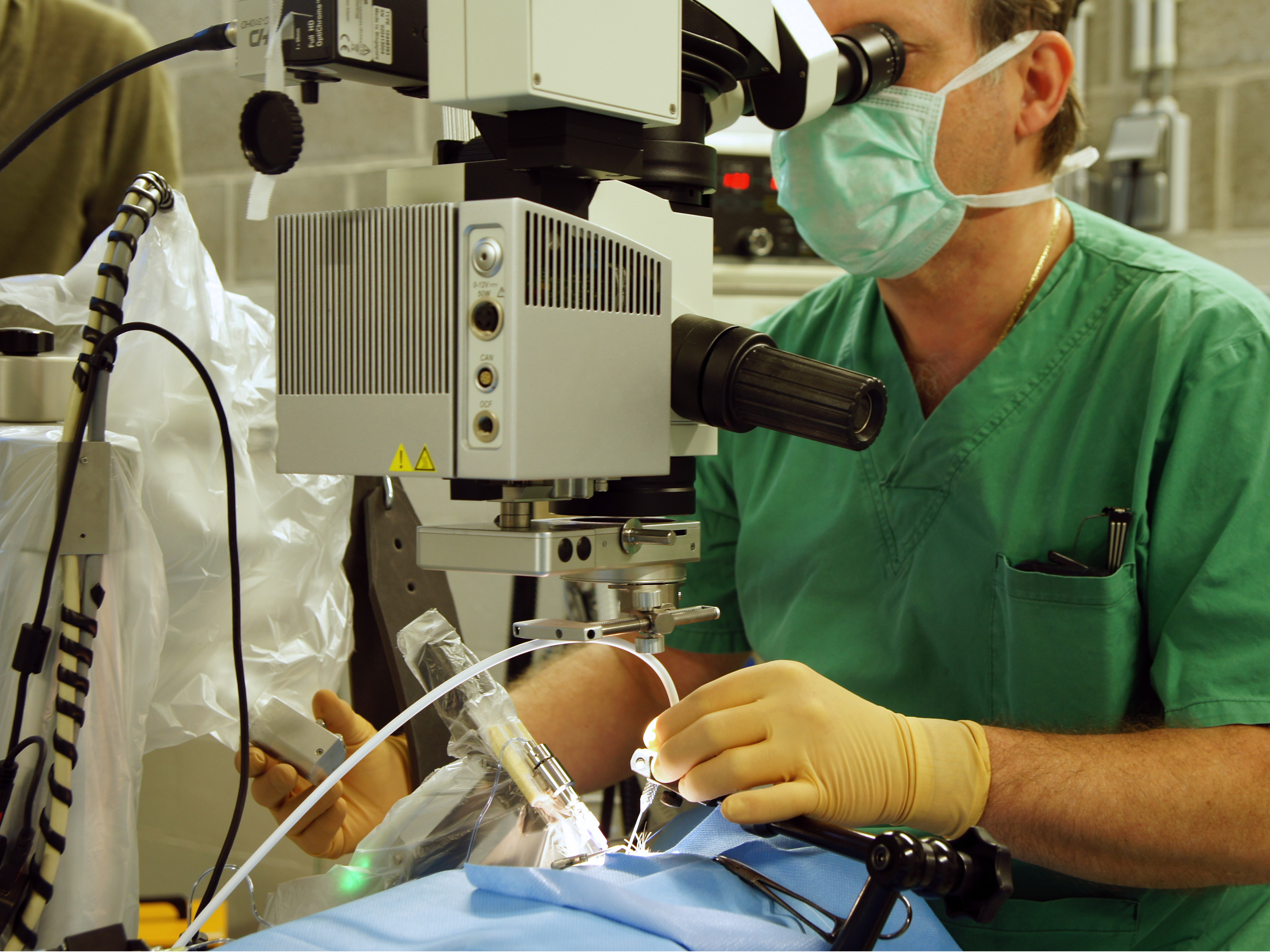
The reason for this is to improve the precision of the movements of the surgical instruments and to impart a stability that is impossible for a human to maintain throughout the course of an arduous and intricate surgical procedure.The PSS has been developed by Dutch company Preceyes, and is being tested and further developed for specific applications in the R2-D2 (an abbreviation for Robotic Retinal Dissection Device) trial, a long-term programme being carried out at the John Radcliffe Hospital in Oxford and in collaboration with Oxford University’s Nuffield Laboratory of Ophthalmology. The trial, which consists of 12 operations, began this year with the first surgery taking place in September. The first phase of the trial, comprising six surgeries, is now complete. Phase two will begin in mid-2017.
The first surgery, which we reported in The Engineer, involved the removal of a membrane around 100µm thick, which had grown over the retina of a 70-year-old man, distorting it and affecting his eyesight. This surgery, the first to be carried out by a robot inside the eye, was performed through a 1mm incision, and the surgical instruments had to be removed and reinserted into this incision several times throughout the surgery, even though, as the patient was under local anaesthetic and conscious throughout, his eyes were moving.
Prof Robert MacLaren, the surgeon in charge of the trials at the John Radcliffe, told The Engineer that the other surgeries in phase one were similar and also included repair of macular holes: tiny holes and tears that can appear in the retina with ageing. Repairing these also involves manipulating membranes on a very small scale inside the eye. Even though ophthalmic surgeons tend to be among the most dextrous of individuals, this type of surgery is extremely difficult because the movements needed inside the eye need to be both precise and controlled. Any hand tremor needs to be eliminated, and surgeons learn to slow their pulse and make the movements needed for the surgery between beats to make sure that there is little chance of even the slightest deviation. The advantage of using the PSS for the surgery is that the intermediary software between joystick and manipulator eliminates those tremors and ensures the movements of surgical instruments are absolutely steady.
“It’s really quite an odd experience at first,” said MacLaren. “I could compare it to driving a car, and then switching to controlling it using your smartphone rather than using the wheel and pedals. In theory, of course, you know it would work perfectly well, but when you actually do it, because you’ve been doing it manually for so long and you’re suddenly relying on computer assistance to help you, it just feels a bit strange. But to go back to the car analogy, you would find that the ride is smoother, you’re going round corners with more stability and there are generally less bumps, and you find that you’re more comfortable with it. As I got more experience with the robotic system it became much more natural. It’s certainly been a most positive experience or I wouldn’t have used it, and I’ve used it several times now.”
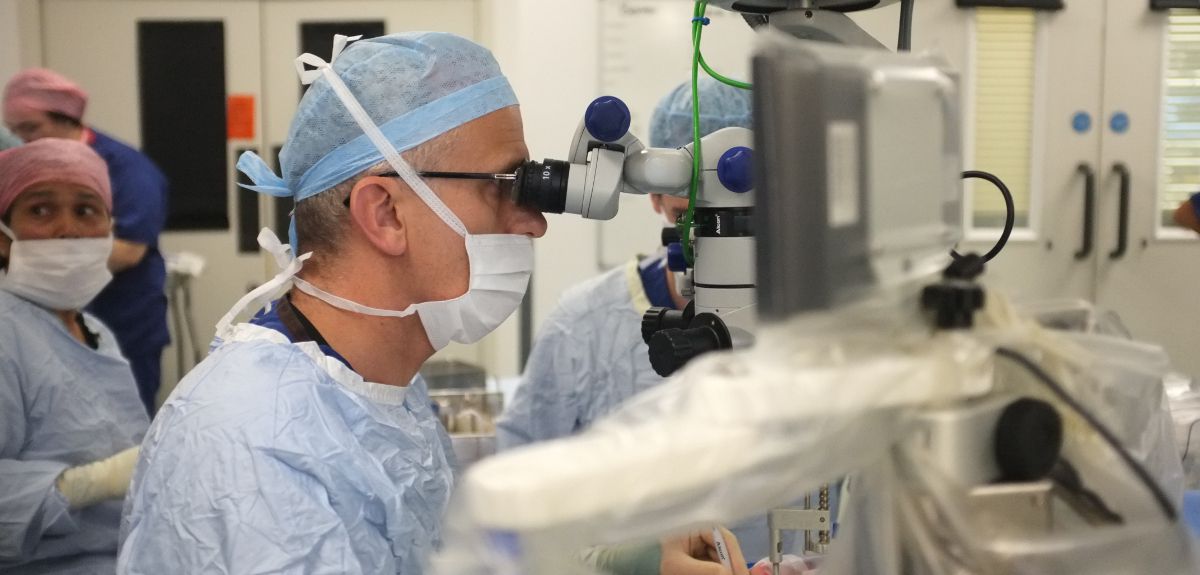
The Preceyes surgical system was initially developed as a collaboration between a mechatronics specialist and an eye surgeon. Gerrit Naus, chief operating officer of Preceyes, explained: “[Eye surgeon] Prof Marc de Smet, who is now our chief medical officer, was professor at Amsterdam Medical Centre, and he met [mechatronics specialist] Prof Maarten Steinbuch, who is a professor at Eindhoven University of Technology and is now also our technical adviser, and they together wrote a project proposal that was granted to build such a robot. The actual research project started about 10 years ago. Then, in 2012, we decided to build a company to fight blindness, and as part of that goal we wanted to take this proof of principle to a proof of concept that we could test in a clinical setting; that’s how we have spent the last four to five years, to develop this actual clinical device that has been tested extensively in our labs and is in use right now in Oxford. It’s an important milestone towards our goal.”
The link with Prof MacLaren started when Preceyes won an innovation award at a major ophthalmology conference and exhibition in 2014, and MacLaren came second with his proposal to use gene therapy to treat eye disorders. ”Of course our team already knew him,” Naus said. “But that was a good point to start discussions. He said: ‘I’m doing this gene therapy trial, but it’s very difficult by hand and maybe you can help me.’ Within a couple of months he had visited our laboratory and was very impressed, and a few months after that we had a contract with a company called Nightstar, which is developing a gene therapy.”

Gene therapy is very suited to robotic surgery in this case, MacLaren explained, because of the stability issue. “The very best ophthalmic surgeons can maybe hold an instrument perfectly still inside the eye for about a minute,” he said. “But after that, your back starts to hurt and you get achey and uncomfortable, and you are naturally going to start to get a bit of a wobble in the instrument. In gene therapy, we want to lift the retina in a controlled way and deliver the active ingredient by injecting it in a very slow way over perhaps 20 minutes. The robot will give us that stability; not just in the precise movements but also in being able to keep absolutely still.”
Moreover, there is a definite need for gene therapies in ophthalmic conditions. Nightstar, the company with which Preceyes is collaborating, is developing a therapy for a disease called choroideremia, an inherited condition in which the light-sensitive cells of the retina degenerate. Inserting a correct version of the gene responsible could help to restore vision. Other eye disorders, also believed to be caused by faulty genes and currently with no treatment, are under investigation for gene therapy. “Right now, gene therapy is not an established therapeutic procedure,” Naus said, “so there are many life science companies that are working on this, and other types of drug-delivery procedures. Surgeons need support administering these drugs at high reproducibility. We are helping them to get the drugs and the right dosage to the right target.”
In fact, it could be said that the existence of the robots such as the PSS is a key reason that these targeted drug-delivery therapies are being developed at all. Naus said it’s not so black and white, but added that Preceyes sees it as a beachhead into general ophthalmic surgery.
Naus is reluctant to reveal many technical details about the robot, but its arm and manipulator hand are controlled by seven motors within the body of the robot. One important difference from machines such as da Vinci is that the surgeon is at the site of the operation and not in a remote room. MacLaren added that this would not be practical for ophthalmic surgery in any case.
“You could probably do it, but I certainly wouldn’t want to,” he said. “When the patient is under local anaesthetic and conscious, you need to talk to them during the operation to put them at ease, relax them and calm them down. Eye surgery is quite a scary thing to undergo. I often tell my residents [junior surgeons] and assistants that most of the anaesthetic my patients need comes out of my mouth. I don’t think you’d want the robot just sitting there above the patient with a needle; there’s a human factor that you really must not neglect.”
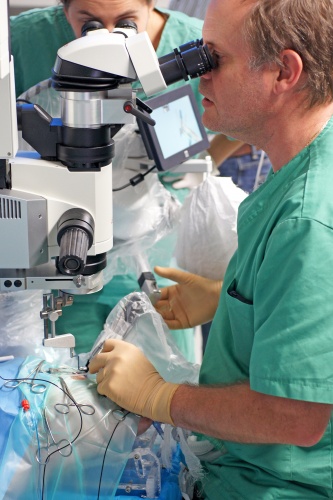
Among the systems incorporated into the PSS to help the surgeon is an ability to switch quickly between assisted surgery and manual, and a function to scale the movement of the manipulator inside the eye. “When you’re in the eye, you want to move very, very slowly. You would maybe want the manipulator to move a hundredth of the distance that you move the joystick, but when you’re outside the eye you want to get away very fast, so the computer will change the scale,” Naus said. MacLaren confirmed that this scaling is invaluable during surgery. He also found a movement limiter to be very useful. “When you first go into the eye, and using the scaled movement you reach a point beyond which you do not want the instrument to go, you press a button on the console and that sets a hard limit so when you go back in you can’t move beyond that point. You don’t feel any resistance on the joystick, but that doesn’t matter because you are always within a safe limit.”
Previous studies with other types of surgical robot have shown a correlation between surgical ability and frequent playing of computer games. Naus is quick to point out that the robot console is not a gamepad but has been specifically designed for this kind of surgery. MacLaren admits to playing PlayStation games with his children, but he didn’t think that this experience was much help. “But eye surgeons tend to have very good manual dexterity. Some of my senior colleagues do watchmaking, and painting and sculpture is common,” he said. “I think generally being used to operating inside the eye is probably a much more relevant thing.”
However, MacLaren does admit that other parts of the system have similarities with computer gaming. For example, he uses virtual reality when observing the operating site through a head-up display connected to a microscope, which also displays additional graphics to assist with the operation. “We do need those extra optics,” he said.
Phase one of the R2-D2 trial was mainly aimed at proving that PSS was safe to use in eye surgery and that it did assist the surgeon in carrying out his or her task. In phase two, MacLaren’s team will be injecting therapeutic agents (drugs in this case, not gene therapy) under patients’ retinas. “It’s a fairly simple procedure, and we are used to doing it, but it will pave the way for the more difficult gene therapy technique,” MacLaren said.




Plasma technique converts landfill methane to jet fuel
Trevor; there are still many landfill sites in the UK where the methane is not captured but not only that, where there is protein waste in them, they...