The bandage, developed by researchers from the University of Nebraska-Lincoln, Harvard Medical School and MIT, can be individually loaded with antibiotics, tissue-regenerating growth factors, painkillers or other medications.
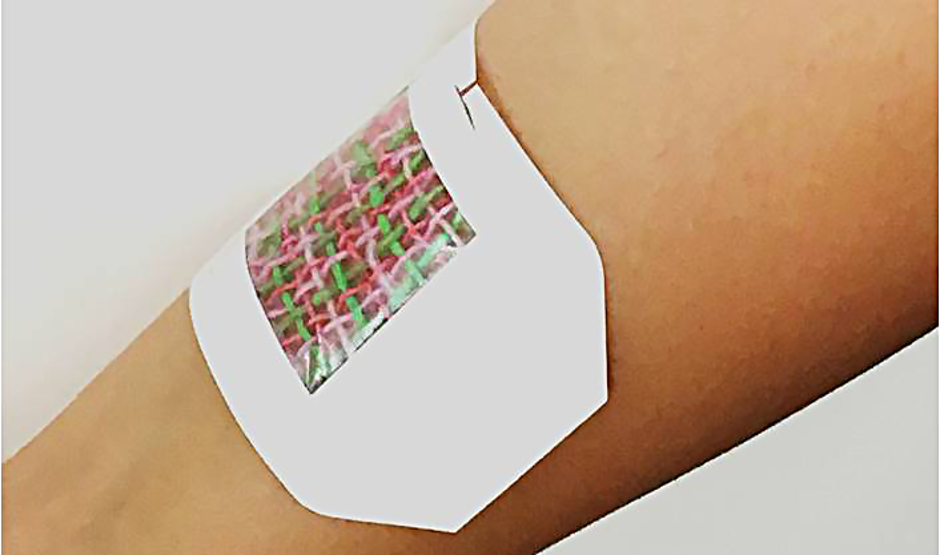
A postage stamp-sized microcontroller, which could be activated by a smartphone or other wireless device, sends small amounts of voltage through a chosen fibre. That voltage heats the fibre and its hydrogel, releasing the medication contained within it.
A single bandage could reportedly accommodate multiple medications tailored to a specific type of wound, the researchers said, while offering the ability to precisely control the dose and delivery schedule of those medications. That combination of customisation and control could substantially improve or accelerate the healing process, said Ali Tamayo, assistant professor of mechanical and materials engineering at Nebraska.
"This is the first bandage that is capable of dose-dependent drug release," Tamayol said in a statement. "You can release multiple drugs with different release profiles. That's a big advantage in comparison with other systems. What we did here was come up with a strategy for building a bandage from the bottom up.
"This is a platform that can be applied to many different areas of biomedical engineering and medicine."
The team envisions its bandage being used initially to treat chronic skin wounds that stem from diabetes. Similarly, those wounded in combat might also benefit from the bandage's versatility, Tamayol said, whether to stimulate faster healing of bullet and shrapnel wounds or prevent the onset of infection in remote environments.
"Soldiers on the battlefield may be suffering from a number of different injuries or infections," he said. "They might be dealing with a number of different pathogens. Imagine that you have a variable patch that has antidotes or drugs targeted toward specific hazards in the environment."
Existing bandages range from basic dry patches to more advanced designs that can passively release an embedded medication over time. To evaluate the potential advantages of their smart bandage, Tamayol and his colleagues at Harvard ran a series of experiments.
In one, the researchers applied a smart bandage loaded with growth factor to wounded mice. When compared with a dry bandage, the team's version regrew three times as much of the blood-rich tissue critical to the healing process.
Another experiment showed that an antibiotic-loaded version of the bandage could eradicate infection-causing bacteria. Collectively, Tamayol said, the experiments also demonstrated that the heat needed to release the medications did not affect their potency.
Though the researchers have patented their design, it will need to undergo further animal and then human testing before the product goes to market.
The team is also working to incorporate thread-based sensors that can measure glucose, pH and other health-related indicators of skin tissue. Integrating that capability would allow the team to create a bandage that could autonomously deliver treatments.
The authors detailed their design and findings in the journal Advanced Functional Materials.

Poll: Should the UK’s railways be renationalised?
I think that a network inclusive of the vehicles on it would make sense. However it remains to be seen if there is any plan for it to be for the...