In type I diabetes, the sufferer's body completely loses its ability to produce insulin, because – for still unknown reasons – the immune system destroys the clusters of cells in the pancreas, known as islets, which produce the hormone. While most diabetics inject insulin several times a day to manage their blood-sugar levels, there has been some investigation of transplanting healthy islets. But so far, this has required subsequent treatment with powerful immunosuppressive drugs, which have unpleasant side effects.

Researchers at Cornell University in New York State are investigating whether the immune system can be tricked into ignoring the transplanted islets by coating them with a protective layer of a hydrogel polymer. Such an approach has previously been discounted because hundreds of thousands of cells need to be implanted to produce an effective reservoir of insulin production, and the encapsulated cells cannot be removed if they fail or die. If this happens, the transplants can generate tumours. “When they fail or die, they need to come out,” said research leader Minglin Ma of the department of biological and environmental engineering. “You don't want to put something in the body that you can’t take out. With our method, that’s not a problem.”
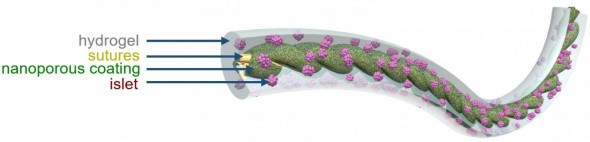
In a paper in the Proceedings of the National Academy of Sciences, Ma explains how the team was inspired by the ability of spider silk to generate beads of water along its length to develop a polymer thread onto which islet cells encapsulated inside hydrogel can be attached. Dubbed TRAFFIC (Thread-Reinforced Alginate Fibre For Islets enCapsulation), the thread is in fact a nanoporous polymer that releases calcium ions, designed so that in alginate, hydrogel will attach strongly to it.
The thread actually performs even better than spider silk, Ma claimed. “You don't have any gaps between capsules,” he said. “With a spider’s silk, you still have gaps between the water beads. In our case, gaps would be bad in terms of scar tissue and the like.”
The team envisages a therapy that would involve the implantation of 6ft of the thread into a patient’s peritoneal cavity. In its paper, the team describes tests on mice using both rat and human islets, and also scaled up the test for implantation and retrieval from dogs; this proved that both surgeries can be carried out using a minimally invasive laparoscopic procedures. TRAFFIC has already received patent protection with the help of Novo Nordisk, the Danish pharmaceutical company that developed injectable insulin some 90 years ago and was a collaborator in the research.




Poll: Should the UK’s railways be renationalised?
All public service companies should be nationalised for many different reasons, particularly railways, not the least because the tax payer has already...