You might not have heard of it, but mention the word Ebola in various parts of Uganda – and indeed anywhere in rural Africa – and the reaction is stark. At times, doctors refuse to see patients with suspected cases. All of a sudden, everyone worries they’ve got it. Queues outside the special clinics and health centres double, then triple. Panic ensues.
None of this is surprising when you learn that Ebola is a deadly and highly contagious virus. The disease it causes, alongside an acute hemorrhagic fever, kills people in a matter of days. The body shuts down from the inside as the symptoms – vomiting, headache, joint pain, diarrhoea – quickly take hold. The worst cases bleed from their nose, eyes, mouth. Of those diagnosed with the airborne strain, 80-90 percent typically succumb.
Although Ebola – possibly transmitted in the faeces of bats and by eating monkey meat – is not common, a suspected case is still alarming for any village. It needs to be contained quickly, patients need to be identified and isolated and people need to be reassured.
As a humanitarian engineer specialising in water and sanitation for the medical charity Médecins Sans Frontières (MSF), Ebola has been my world for the last week. On a trip to north eastern Uganda to deal with a suspected case, I was reminded just how complex a challenge this disease is – and how much we owe to engineering thinking and practice when it comes to containing it.
Initially, Ebola occurred just outside the Ugandan capital Kampala. A middle aged woman died and tests confirmed she had it. The government was very nervous because the disease is so virulent. They called MSF in to tackle a second suspected case in a place called Kabong.
As soon as we arrived we set to work, fully prepared for an Ebola outbreak. Our first hurdle involved ‘line tracing’ all the people the patient had come into contact with in recent hours and days. That meant finding out where the woman had gone as she travelled to the clinic to report her symptoms. We needed to know where she had had dinner, who she had spoken to and if she had stopped on her way.
It seems extreme, but it’s necessary. In typical cases of Ebola, the first people to die are usually the patient, anyone caring for them at home, their doctor and any nursing staff. Containment in the early stages is absolutely critical.
And containment is really what Ebola is all about. So we set about building an isolation ward.
In a rural Ugandan village with limited resources, our choice of building materials was slim. We settled initially for tents, reams of plastic sheeting, wooden poles and tarpaulin.

In fact, the construction of the ward itself is the easy bit. The real conundrum comes when you consider the need to keep each section of the structure (suspected, infected and confirmed cases) isolated from one another.
It’s less to do with construction and more to do with flow; involving basic logistics, planning paths of movement from one room to the next and designing a pre-agreed ‘circuit’ for each health worker and patient to adhere to.
On top of that each family member, doctor, nurse and water and sanitation adviser is necessarily clad in protective clothing from head to toe. Anyone coming into contact with a patient needs to wear green scrub like underwear, overalls, an all-in-one paper suit, goggles, two pairs of gloves and a plastic apron.
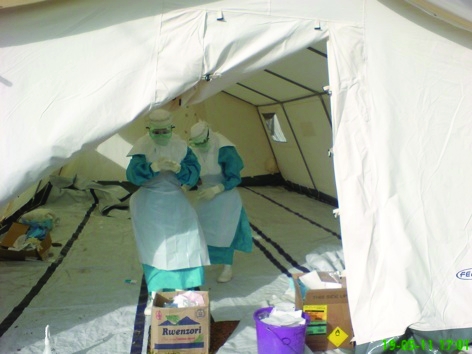
And each time you move from a high risk to a low risk area, you need to get undressed and redressed to stop potential spread of infection. At all stages you are sprayed with a chlorine solution, and each doorway has a chlorine footbath.
Disposing waste is just as challenging. How do you get rid of a bucket of infected fluid when there’s nowhere to put it? Where do you bin used and highly infectious clothing? What about contaminated water used to hose down the sections of the isolation ward? How do you get supplies into and out of the field camp – or simply stop people wandering into the exclusion zone?
Each problem requires its own particular engineering solution. Often the answer involves chlorine – and masses of it. And you quickly become obsessed with detail, constantly thinking about where you’ve been and where you’re going next.
Some solutions are simpler – we used three layers of fencing to block the isolation ward off from passing villagers. Culturally, there are multiple challenges too. Just explaining what you are up to can be tricky enough!
Unfortunately, in this particular case, and despite all of our best efforts, we were unable to save the patient who sadly passed away after just two days. Only after we left did we discover that she had, in fact, not died of Ebola – even though she showed all the symptoms. But we didn’t have the luxury of that knowledge until it was too late. And with Ebola you can’t take any chances.
On the plus side, we left the community with a permanent isolation ward for potential future cases, trained a number of local staff in procedures used to deal with an outbreak and helped protect the villagers of Kabong from what could have been a very deadly situation. Taken together, these measures will save more lives in the years to come. For me, it’s just one example of humanitarian engineering in action.
![]()
To find out more about RedR’s work, visit the website, www.redr.org.uk





Poll: Should the UK’s railways be renationalised?
I _do_ remember British Rail - and that it was <i>literally</i> a national joke https://youtu.be/zV2lmSDKvO8