C2I 2020Category: Covid-19 response
Project: CE Imperial Lather
Partners: Imperial College Essential Staff Team, Department of Chemical Engineering, with Sipsmith London
Alongside pasta and toilet roll, one of the first things to disappear from supermarket shelves in the early days of the pandemic was hand sanitiser. What had been a low-cost, freely available product, became a highly prized and overpriced commodity practically overnight. As consumers scrambled to stock up on the antibacterial gel, hospitals and care homes also began to feel the pinch, struggling to provide staff with an essential tool for preventing COVID transmission.
In response to the shortage and an emergency appeal from the Imperial College Healthcare NHS Trust, a small team of volunteers from Imperial’s chemical engineering department came together to find a solution, sourcing feedstocks for hand sanitiser and establishing a production line. Initially, the team relied on donations of excess ingredients from various other Imperial departments, converting existing undergraduate teaching laboratories into the main production area to manufacture the gel. Once news of the project got out, London gin distillery Sipsmiths got in touch and pledged to provide 10,000 litres of ethanol, a key base component for the production of hand sanitiser.
The Science Museum - located adjacent to Imperial College in South Kensington - then stepped up with a supply of glycerol, another vital ingredient. All that was needed now was a name. If The Engineer was giving awards for the best project title, Imperial Lather would undoubtedly walk away with the Grand Prix. But how to get the fabulously monikered gel out to the frontlines where it was so desperately needed? Lockdown meant that many courier services were cancelled or severely overstretched. Fortunately, one of the team was ADR registered - licensed to transport hazardous goods by road - and the gel was distributed across an 80-mile delivery route using one of Imperial College’s own vans.
CLICK FOR JOINT WINNERS OF COVID-19 RESPONSE
Throughout the early stages of the pandemic, the team sourced, manufactured and distributed thousands of litres of hand sanitiser gel to hospitals and care homes around London. It’s a project that typifies how UK industry has responded to the COVID crisis, and one which had an immediate and important impact on the frontlines of healthcare.
C2I 2020Category: Covid-19 response
Project: 3D printed auxetic nasopharyngeal swabs for COVID-19 sample collection
Partners: University of Wolverhampton with 6DME UK
As anyone who has been tested for COVID-19 over the past year can confirm, having a six-inch swab inserted into the nasal passage does not make for the most pleasant of experiences. This collaboration, led by the University of Wolverhampton, sought not only to reduce the discomfort arising from nasopharyngeal swabs, but to do so using 3D printing and an open-source design that could be replicated anywhere in the world.
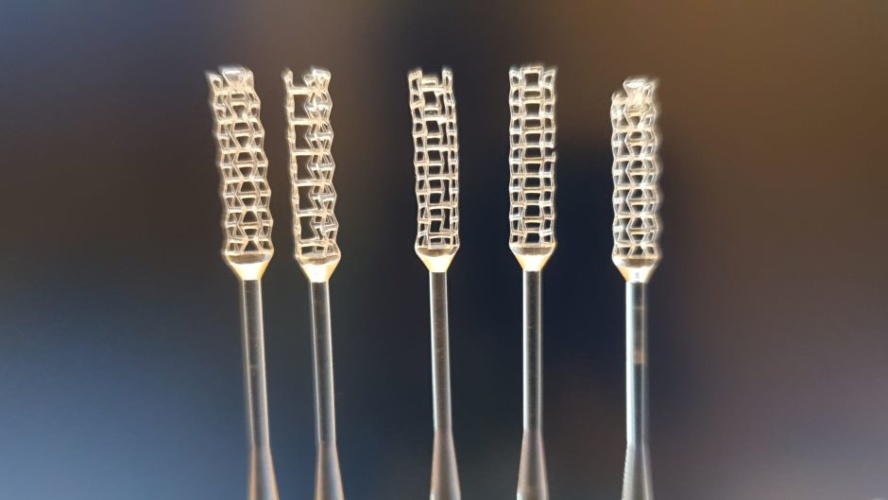
The nasopharyngeal swabs required for the coronavirus tests are different from standard cotton swabs. They are usually 15 cm long with a tip diameter of 0.35-0.40 cm suitable to get to the nasopharynx. According to the guidelines issued by the Centre for Disease Control and Prevention in the US, the swabs should be made of synthetic fibre and not comprise a wooden shaft, as this can interfere with test results. Usually, the nasopharyngeal swabs are inserted through the nostril until they reach the inferior concha and the back of the nasopharyngeal cavity. They are then rotated five times and removed to be analysed, whether locally using lateral flow kits or in the laboratory with PCR (polymerase chain reaction) testing.
Working with 6DME, the Wolverhampton team developed a new self-adjusting 3D printed nasal swab design to mitigate the discomfort of the testing process by shrinking to better fit the patient’s nasal cavity. The partners used computer aided design (CAD), finite element analysis (FEA) and surrogate modelling techniques to develop a metamaterial swab that adapts to the contours of each individual’s nasal passage, putting significantly less stress on the surrounding tissues in comparison to traditional swabs. To ensure that as many people as possible benefit from the research, the team said it will make the design and all accompanying data publicly available so that the swabs can be 3D printed anywhere and on demand.





Hard hat mounted air curtain adds layer of protection
Something similar was used by miners decades ago!