
(Pic: Ian Papautsky)
The device separates the various cell types found in blood by their size and could eventually lead to rapid, cheap liquid biopsies to help detect cancer and develop targeted treatment plans. The findings are reported in Microsystems & Nanoengineering.
"This new microfluidics chip lets us separate cancer cells from whole blood or minimally-diluted blood," said Ian Papautsky, the Richard and Loan Hill Professor of Bioengineering in the University of Illinois at Chicago (UIC) College of Engineering and corresponding author on the paper. "While devices for detecting cancer cells circulating in the blood are becoming available, most are relatively expensive and are out of reach of many research labs or hospitals. Our device is cheap, and doesn't require much specimen preparation or dilution, making it fast and easy to use."
The ability to successfully isolate cancer cells is a crucial step in enabling liquid biopsy where cancer could be detected through a simple blood sample. This would eliminate the discomfort and cost of tissue biopsies which use needles or surgical procedures as part of cancer diagnosis. Liquid biopsy could also be useful in tracking the efficacy of chemotherapy, and for detecting cancer in organs difficult to access through traditional biopsy techniques.
Circulating tumour cells are present in extremely small quantities. For many cancers, circulating cells are present at levels close to one per one billion blood cells. "A 7.5-millilitre tube of blood, which is a typical volume for a blood draw, might have ten cancer cells and 35-40 billion blood cells," said Papautsky. "So, we are really looking for a needle in a haystack."
Microfluidic technologies either use markers to capture targeted cells as they float by, or they take advantage of the physical properties of targeted cells - mainly size - to separate them from other cells present in fluids.
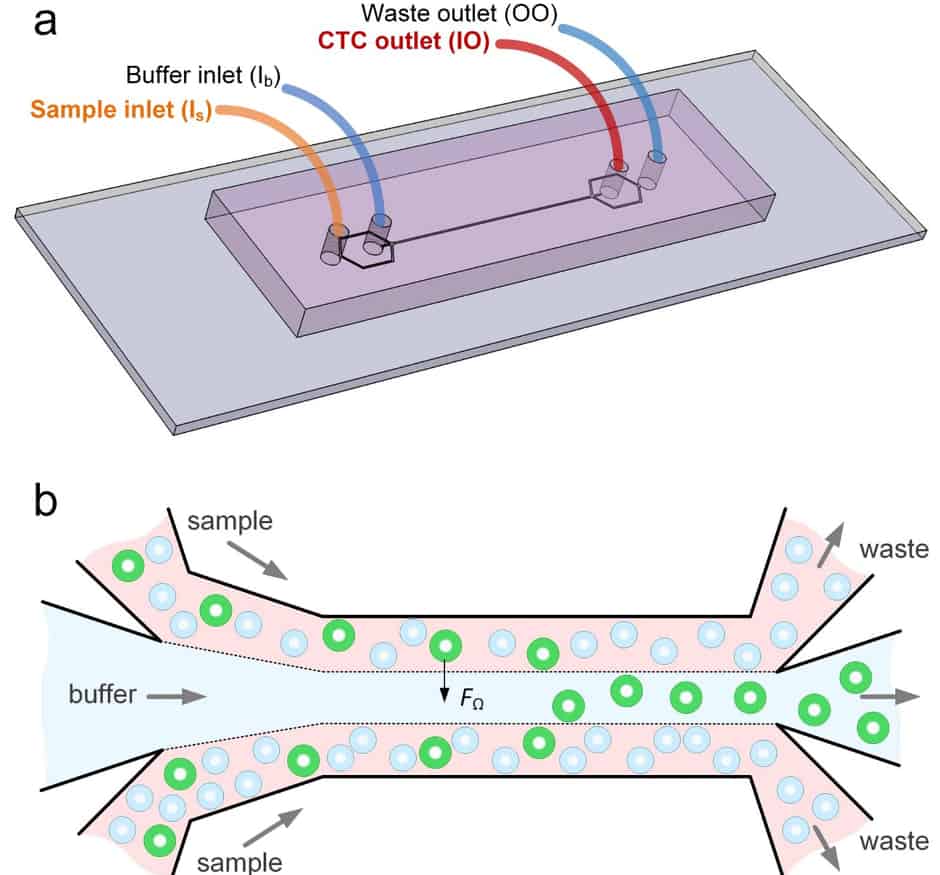
Papautsky and his colleagues at UIC and Queensland University of Technology developed a device that uses size to separate tumour cells from blood. "Using size differences to separate cell types within a fluid is much easier than affinity separation which uses 'sticky' tags that capture the right cell type as it goes by," said Papautsky. "Affinity separation also requires a lot of advanced purification work which size separation techniques don't need."
The device is said to capitalise on the phenomena of inertial migration and shear-induced diffusion to separate cancer cells from blood as it passes through 'microchannels' formed in plastic. "We are still investigating the physics behind these phenomena and their interplay in the device, but it separates cells based on tiny differences in size which dictate the cell's attraction to various locations within a column of liquid as it moves."
Papautsky and his colleagues 'spiked' 5-millilitre samples of healthy blood with 10 small-cell-lung cancer cells and then ran the blood through their device. They were able to recover 93 per cent of the cancer cells using the microfluidic device. Previously-developed microfluidics devices designed to separate circulating tumour cells from blood had recovery rates between 50 per cent and 80 per cent.
When they ran eight samples of blood taken from patients diagnosed with non-small-cell lung cancer, they were able to separate cancer cells from six of the samples using the microfluidic device.




Labour pledge to tackle four key barriers in UK energy transition
I'm all for clarity and would welcome anyone who can enlighten me about what Labour's plans are for the size and scale of this Great British Energy....